If you turn on the television, open a magazine or newspaper, surf the Internet, or scroll through social media in October, it’s pretty much a given that you will hear or read about breast cancer. But how much of what you hear or read is true?

October is Breast Cancer Awareness Month, and it’s a perfect time to learn more about the disease that one out of eight women will get in their lifetimes. However, thanks in large part to the unvetted nature of social media, it’s also a time when misinformation is out there spreading with every click and “like.” Whether you are a survivor, current patient or want to lessen your chances of getting breast cancer, it’s important to know what’s fact and what’s fiction. Here’s the truth about several things that are commonly linked to breast cancer.
Radiation from mammograms
While mammograms do give off low doses of radiation, the benefits of these screenings far outweigh the risks, say experts. Mammograms are the best tool to catch the disease in its early stages, before it’s spread. When caught at Stage I, when it’s localized and hasn’t spread, patients have a 99% five-year survival rate. The risk of annual mammograms possibly causing cancer is 20 to 25 out of every 100,000 women. Yet, one in 69 women will develop breast cancer by age 40, and one in eight will develop the disease in their lifetimes.
“The radiation from mammograms is minimal and mammography is still the best general screening modality,” says Dr. Jessica Bensenhaver, director of the Breast Cancer Program at Henry Ford Cancer Institute in Detroit Mich. “In some cases, for women who are found to be high risk for breast cancer either by mutation or by formal risk assessment, we add MRI to an annual screening. However, even for these patients, mammography is still required as all modalities have limitations and utilizing one doesn’t negate the need for another.”
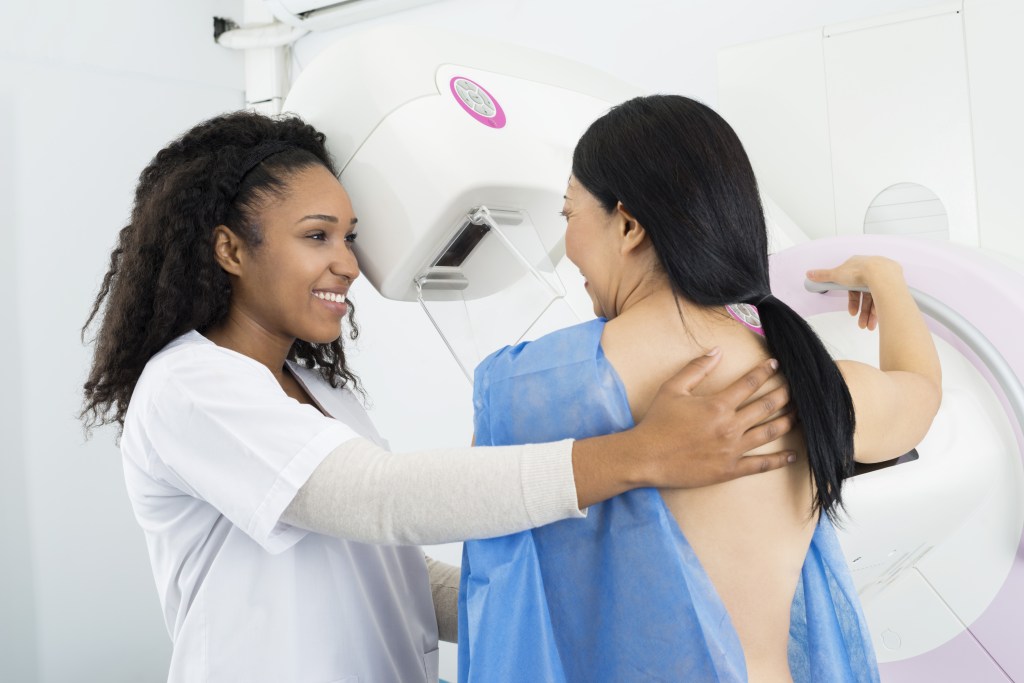
In recent times, thermal imaging, which produces an infrared image that shows the patterns of heat on or near the surface of the body, has been touted as a “safe” alternative to mammograms to screen for breast cancer because it doesn’t use radiation. The FDA has advised against using thermal imaging to detect breast cancer. You should never use thermography in place of mammograms, according to Dr. Ruth Lerman, a specialist in breast health and disease for Beaumont Health, in Southfield, Mich. “They are horrible,” she says. “They give false positives, they give false negatives, and they have given people a false sense of security who had masses. They are a waste of money.”
Bottom line: If you are at average risk and 40 or older, talk to your doctor about when you should get a mammogram.
Hormonal birth control
Most studies have shown taking hormonal contraception raises your risk for getting breast cancer, but only slightly, and that risk goes away eventually once it’s stopped.
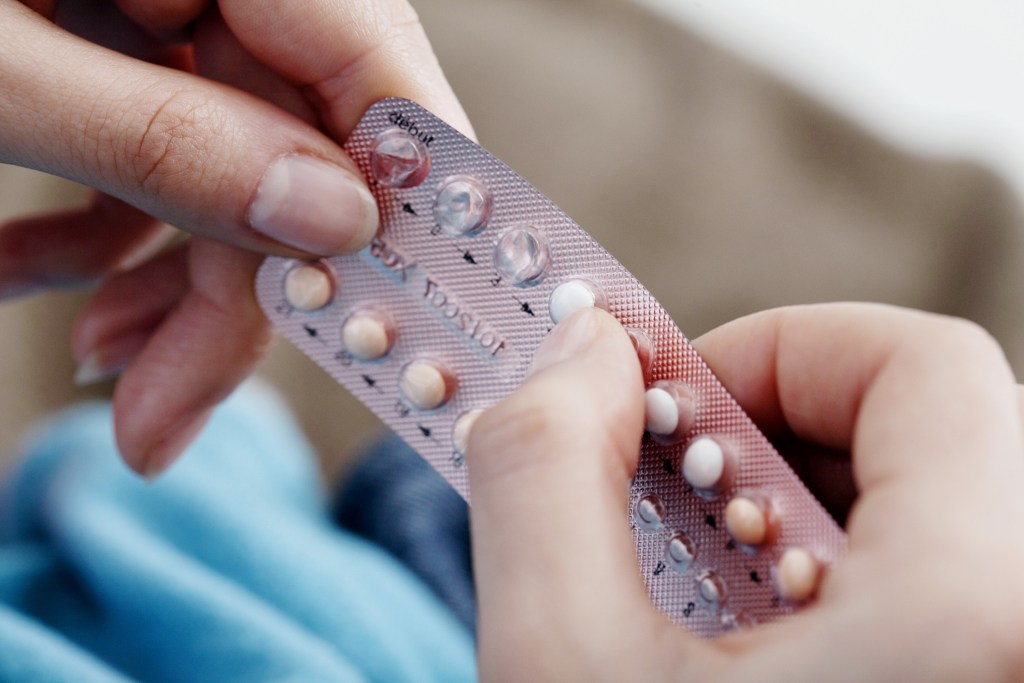
A large recent Danish study found that women who had recently or currently used newer, low-dose combination oral contraceptives (pills containing estrogen and progesterone) had a 20% increase in breast cancer risk compared to those who had never taken hormonal contraceptives. The study found that the increased breast cancer risk went down rapidly for those who discontinued oral contraceptives after short-term use, while increased risk could remain for five years or more after stopping usage for women who had taken oral contraceptives for longer periods of time. Researchers added that the study’s results indicated only a slightly higher breast cancer risk for women who’d used hormonal contraception than for those who hadn’t.
There have been few studies on the link between progestin-only pills and breast cancer. A recent large study found that the use of Mirena, a levonorgestrel-releasing intrauterine device, or IUD, also increased breast cancer risk by about 20%. However, using Mirena was associated with a lower risk of endometrial and uterine cancers.
If you’re on or considering using hormonal birth control, experts say it’s important to talk to your doctor and weigh the risks versus the benefits.
Hormone replacement therapy
Commonly known as HRT, this therapy is often used by perimenopausal and post-menopausal women to combat symptoms such as hot flashes, mood swings, and sleep disturbances. The link between using combined estrogen/progesterone HRT and increased breast cancer risk is well established by research, according to Lerman. “There is a clear and strong association between using combined estrogen and progesterone hormone replacement therapy and increased breast cancer risk after menopause,” she says.
While studies have shown conflicting results about increased risks for postmenopausal women without uteruses who take estrogen-only hormone therapy, any type of HRT with estrogen represents a risk, according to Bensenhaver. “HRT in general, whether a combination or single agent, is going to increase your risk,” she says. “Basically, if you are exposed to exogenous estrogen or estrogen-like substances, there is going to be a risk.”
Discontinuing HRT use was found to lessen, but not erase, increased breast cancer risk. It should be noted that the vast majority of studies on HRT and breast cancer have been done on synthetic hormones, which are derived from manmade chemical compounds or, in the case of the estrogen-replacement Premarin, urine from pregnant horses. Little research has been done into breast cancer risk and the use of bioidentical hormone therapy, or BHRT, which uses estrogen and/or progesterone synthesized from plants to create compounds molecularly identical to hormones the body produces. Advocates tout BHRT as a safer alternative to synthetic hormones; the research that has been done on BHRT has produced conflicting results.
Lerman’s advice on any type of HRT: “Use the lowest possible dose for the shortest time possible for symptoms to be manageable. When you get off of it, the risk goes down, and many women who needed it when they first developed symptoms find they can later taper off,” she says.

Antiperspirants with aluminum
Talk of aluminum in antiperspirants possibly causing breast cancer has gained a lot of traction in recent times, and no doubt in some part spurred the increasing number of non-aluminum “natural” deodorants hitting the marketplace. You might have heard that the aluminum in antiperspirant plugs the underarm sweat glands and causes toxins to accumulate. Or maybe you’ve read that the aluminum itself can cause cancer when it’s absorbed into the body’s lymph nodes through the underarms.
While these notions have often been dismissed by medical experts, a recent study published in The Lancet comparing underarm cosmetic product use and aluminum measurements in breast cancer patients and healthy individuals had some interesting results. The study’s findings suggested that frequently using antiperspirants could lead to aluminum accumulating in the breast tissue and that using the products more than once daily may increase breast cancer risk in young women. The study’s authors recommended that particularly women at younger ages should be careful and avoid excessive use of antiperspirants with aluminum until more definitive answers can be found.
If you are concerned but don’t want to give up your antiperspirant, Lerman suggests not using the products right after shaving, which causes very small nicks in the skin. “A sensible approach is don’t put it on right after shaving your armpits, which impairs the barrier that the skin provides,” she says. “If you are worried, shave at night and put your deodorant on in the morning.”
Plastic bottles and containers
When musician Sheryl Crow was diagnosed with breast cancer in 2006, she speculated that drinking from plastic water bottles that she’d left in hot cars might have caused her disease. While it’s not always easy to pin down an exact cause of cancer (and often there can be many factors at work), there is evidence of a link between the plastic used in water bottles and breast cancer.
Bisphenol A, or BPA, a chemical substance used in plastic bottles and food storage containers, is proven to be a hormonal disruptor, and there is a suggested association between increased breast cancer incidence and exposure to BPA at levels below those considered environmentally safe. These effects are thought to be exacerbated when plastics are heated, which can cause chemicals to leech into food and liquids.
“There is definitely a concern about plastics because they’re endocrine disruptors,” says Lerman. “My advice is don’t put any plastic in the microwave, meaning containers or covering food in plastic. Avoid canned goods, which often have BPA in the lining. Instead, use products that are in glass or frozen.”

Carrying your cell phone in your bra
The dangers of touting your cell phone in your bra ran rampant several years ago after The Dr. Oz Show featured a guest who said that carrying her cell phone that way for four years led to her diagnosis of breast cancer at a very young age. Most studies have looked at the link between radiofrequency radiation from cell phones and brain tumors. However, a recent case study of four young women with breast cancer brought “forth the possibility of a relationship between prolonged direct skin contact with cellular phones and the development of breast cancer,” according to the study’s authors. This was a very small study, and researchers concluded that more studies need to be done.
The American Cancer Society states that it does not have any official position or statement on whether or not radiofrequency radiation from cell phones, cell phone towers, or other sources is a cause of cancer. Based on a review of studies, the International Agency for Research on Cancer has classified radiofrequency radiation as “possibly carcinogenic to humans,” based on “limited evidence of a possible increase in risk for brain tumors among cell phone users, and inadequate evidence for other types of cancer.”
It’s fair to say the jury is still out on the risk of carrying cell phones close to your heart — or breasts. In this case, you might want to go with “better safe than sorry,” and tote your phone in your purse.
BlissMark provides information regarding health, wellness, and beauty. The information within this article is not intended to be medical advice. Before starting any diet or exercise routine, consult your physician. If you don’t have a primary care physician, the United States Health & Human Services department has a free online tool that can help you locate a clinic in your area. We are not medical professionals, have not verified or vetted any programs, and in no way intend our content to be anything more than informative and inspiring.




